
What is polycystic ovary syndrome (PCOS)?
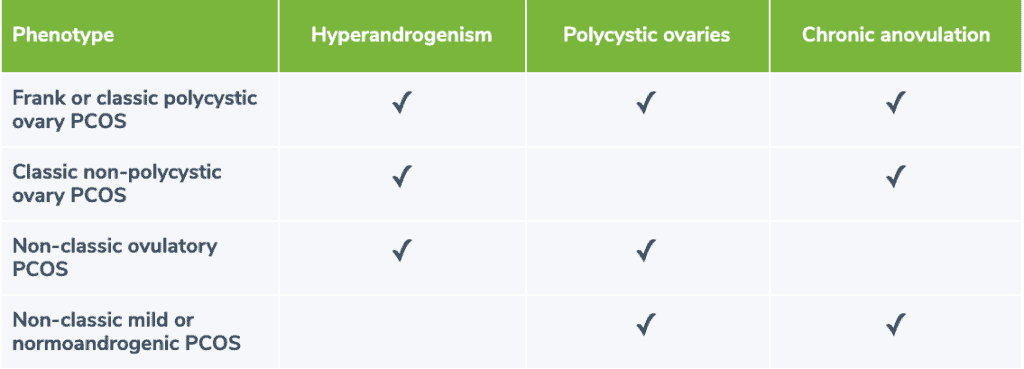
PCOS is a complex endocrine disorder that involves excess androgen (hyperandrogenism), menstrual irregularity, and/or polycystic ovaries. (3)(12) PCOS is typically characterized by high circulating levels of certain hormones (e.g., testosterone, androstenedione, luteinizing hormone), as well as 12 or more follicles between 2-9mm in diameter in each ovary and/or an ovarian volume exceeding 10ml. (3) The clinical presentation of PCOS may vary, however the Rotterdam criteria, one set of guidelines for PCOS diagnosis, divides the condition into the following four phenotypes:- Frank or classic polycystic ovary PCOS: characterized by hyperandrogenism, polycystic ovaries, chronic anovulation, and poor metabolic and cardiovascular risk factor profiles (e.g., insulin resistance, lipid profile) compared to non-classic phenotype
- Classic non-polycystic ovary PCOS: characterized by hyperandrogenism and chronic anovulation, but ovaries are normal/non-polycystic
- Non-classic ovulatory PCOS: characterized by hyperandrogenism and polycystic ovaries, but menstrual cycles are regular
- Non-classic mild or normoandrogenic PCOS: characterized by chronic anovulation and polycystic ovaries, but androgens are normal (3)
Signs, symptoms, and comorbidities
PCOS typically presents with a variety of symptoms associated with excess androgen and menstrual dysfunction, (3) including:- Acanthosis nigricans (dark, velvety patches on the skin)
- Acne
- Alopecia and androgenetic alopecia (hair loss)
- Anovulation
- Amenorrhea
- Hirsutism (excessive hair growth, particularly on the face, chest, and back)
- Oligomenorrhea
- Pelvic pain (10)(3)(12)
- Skin tags

- Cancer (e.g., endometrial)
- Cardiovascular disease (CVD)
- Dyslipidemia
- Fatty liver
- Infertility or subfertility
- Insulin resistance
- Metabolic syndrome
- Obesity
- Psychological disorders (e.g., depression, anxiety, substance abuse, disordered eating, psychosexual dysfunction)
- Sleep apnea
- Type II diabetes (3)(6)(12)(10)
PCOS causes and risk factors
PCOS involves dysfunctions in ovarian function, insulin metabolism, and hypothalamic-pituitary axis function. While the cause of PCOS is unknown, the condition is believed to develop as a result of a combination of genetic and environmental factors. (6)(12) Some identified risk factors include:- Diabetes and insulin resistance
- Family history
- Inactivity, sedentary lifestyle
- Infectious agents and toxins
- Obesity
- Poor dietary choices (6)(12)
Ingredients for PCOS
PCOS treatment typically involves the collaboration of an interdisciplinary team and a combination of lifestyle (e.g., diet, exercise) and pharmaceutical interventions (e.g., insulin-sensitizing agents). Commonly prescribed medications include metformin, thiazolidinediones, and spironolactone. (3) Certain dietary supplements have also been shown to be effective in supporting the treatment of PCOS.Berberine
Berberine is the primary active component of several medicinal herbs, including Berberis vulgaris (barberry), Coptis chinensis (Chinese goldthread), Phellodendron amurense (Amur corktree), and Hydrastis canadensis (goldenseal). (10)(12) Berberine has been used traditionally in the treatment of a number of conditions, including gastrointestinal conditions (e.g., diarrhea), metabolic conditions, and infertility. Recently, berberine has been used to enhance the effectiveness of certain medications, namely cyproterone acetate (CPA), clomiphene (CC), and letrozole (LET). Berberine supplementation has also been shown to reduce insulin resistance, improve cholesterol levels, and decrease waist circumference and waist-to-hip ratio. (10)(14) Further research has demonstrated the effectiveness of berberine supplementation in reducing some of the negative effects of PCOS, including total testosterone, free androgen index, fasting glucose, and insulin. (1)(15)
D-chiro-inositol and myo-inositol
An important component of cell membranes, D-chiro-inositol (DCI), and myo-inositol (MI) are the two most abundant inositols of the inositol stereoisomer family. MI and DCI are found abundantly in nature, particularly in fruit and beans. The effectiveness of MI and DCI in PCOS is believed to be attributed to their role in ovarian function and in maintaining normal levels of hormones, such as insulin and follicle-stimulating hormone (FSH). Imbalances or deficiencies in MI and DCI have been shown to contribute to PCOS. Therefore, correcting these imbalances through supplementation may help address the features and symptoms of the condition. (9) Research has demonstrated that DCI may improve acne, menstrual cycle regularity, and insulin resistance in young PCOS patients. (5) DCI supplementation also demonstrated effectiveness in improving ovarian function and metabolism in patients with PCOS. (13) A meta-analysis demonstrated that MI improves the homeostatic model assessment (HOMA) of insulin resistance and increases E2 (estradiol) levels. These results suggest that MI may be beneficial for the treatment of PCOS with insulin resistance and may help improve symptoms associated with decreased estrogen. (16) MI has also been shown to significantly decrease serum total testosterone, modified Ferriman-Gallwey (mF-G) scores, and serum high-sensitivity C-reactive protein (hs-CRP) levels (7)Chromium picolinate
Chromium is a trace mineral found in small amounts in a wide variety of dietary sources, including meat, whole grains, and some vegetables, fruit, and spices. Unfortunately, dietary intake of chromium is difficult to determine as it is significantly affected by agricultural and manufacturing processes. Chromium is found in two primary forms, biologically active trivalent chromium found naturally in food and toxic hexavalent chromium, a bi-product of industrial pollution. (11) Trivalent chromium (Cr3+) can also be obtained in various supplemental forms, the most popular being chromium picolinate which contains 12.4% elemental trivalent chromium. (2) Chromium has been shown to improve insulin sensitivity, (8) BMI, testosterone concentrations, cardiometabolic risk factors, and oxidative stress in cases of PCOS. (4)The bottom line
PCOS is a complex endocrine disorder commonly treated with lifestyle and pharmaceutical interventions. Research has shown that certain dietary supplements, including berberine, D-chiro-inositol, myo-inositol, and chromium, may be beneficial for individuals with PCOS. A protocol using natural supplements can be used therapeutically on its own or as an adjunct to existing treatment. If you’re a patient, we recommend speaking with your healthcare provider to find out if these supplements are right for your wellness plan. If you’re a practitioner, view our ovarian wellness protocol.- An, Y., Sun, Z., Zhang, Y., Liu, B., Guan, Y., & Lu, M. (2014). The use of berberine for women with polycystic ovary syndrome undergoing IVF treatment. Clinical Endocrinology, 80(3), 425-31.
- Ashoush, S., Abou‐Gamrah, A., Bayoumy, H., & Othman, N. (2016). Chromium picolinate reduces insulin resistance in polycystic ovary syndrome: Randomized controlled trial. The Journal of Obstetrics and Gynaecology Research, 42(3), 279-285.
- El Hayek, S., Bitar, L., Hamdar, L. H., Mirza, F. G., & Daoud, G. (2016). Polycystic ovarian syndrome: An updated overview. Frontiers in Physiology, 7, 124.
- Fazelian, S., Rouhani, M.H., Bank, S.S., & Amani, R. (2017). Chromium supplementation and polycystic ovary syndrome: A systematic review and meta-analysis. Journal of Trace Elements in Medicine and Biology, 42, 92-96.
- Formuso, C., Stracquadanio, M., & Ciotta, L. (2015). Myo-inositol vs. D-chiro inositol in PCOS treatment. Minerva Ginecologica, 67(4), 321-5.
- Genetics Home Reference. (2019). Polycystic ovary syndrome. Retrieved from https://ghr.nlm.nih.gov/condition/polycystic-ovary-syndrome
- Jamilian, M., Farhat, P., Foroozanfard, F., Afshar Ebrahimi, F., Aghadavod, E., Bahmani, F., … Asemi, Z. (2017). Comparison of myo-inositol and metformin on clinical, metabolic and genetic parameters in polycystic ovary syndrome: A randomized controlled clinical trial. Clinical Endocrinology, 87(2), 194-200.
- Jamilian, M., Zadeh Modarres, S., Amiri Siavashani, M., Karimi, M., Mafi, A., Ostadmohammadi, V., & Asemi, Z. (2018). The influences of chromium supplementation of glycemic control, markers of cardio-metabolic risk, and oxidative stress in infertile polycystic ovary syndrome women candidate for in vitro fertilization: A randomized, double-bling, placebo-controlled trial. Biological Trace Element Research, 185(1), 48-55.
- Kalra, B., Kalra, S., & Sharma, J. B. (2016). The inositols and polycystic ovary syndrome. Indian Journal of Endocrinology and Metabolism, 20(5), 720–724.
- Li, M., Zhou, X., & Li, X. (2018). The effect of berberine on polycystic ovary syndrome patients with insulin resistance (PCOS-IR): A meta-analysis and systematic review. Evidence-Based Complementary and Alternative Medicine.
- National Institutes of Health. (2019). Chromium. Retrieved from https://ods.od.nih.gov/factsheets/Chromium-HealthProfessional/
- Ndefo, U. A., Eaton, A., & Green, M. R. (2013). Polycystic ovary syndrome: A review of treatment options with a focus on pharmacological approaches. Pharmacy & Therapeutics, 38(6), 336–355.
- Pizzo, A., Laganà, A., & Barbaro, L. (2014). Comparison between effects of myo-inositol and D-chiro-inositol on ovarian function and metabolic factors in women with PCOS. Gynecological Endocrinology, 30(3), 205-8.
- Wang, Y., & Zidichouski, J. A. (2018). Update on the benefits and mechanisms of action of the bioactive vegetal alkaloid berberine on lipid metabolism and homeostasis. Cholesterol, 2018, 7173920.
- Wei, W., Zhao, H., Wang, A., Sui, M., Liang, K., Deng, H. , … Guan, Y. (2012). A clinical study on the short-term effect of berberine in comparison to metformin on the metabolic characteristics of women with polycystic ovary syndrome. European Journal of Endocrinology, 166(1), 99-105.
- Zeng, L., & Yang, K. (2018). Effectiveness of myoinositol for polycystic ovary syndrome: A systematic review and meta-analysis. Endocrine, 59(1), 30-38.





