Currently, more than half of reproductive-aged women in the United States are using contraception. (8) The birth control pill, also known as oral contraceptives or simply “the pill”, is a hormonal pharmaceutical medication taken daily as a method to prevent pregnancy and provide menstrual regularity. (7) As a medication, significant research has been conducted to investigate the physiological changes that can occur in women taking the pill. (25) If you have been prescribed an oral contraceptive by your healthcare practitioner, it’s important to be mindful of contraindications and potential nutrient depletions that may occur.
Continue reading to learn more about various forms of contraception and important considerations when taking the birth control pill.
What is birth control?
Birth control, another word for contraception, encompasses any method used to prevent pregnancy.
Pregnancy begins at conception, when fertilization occurs and a developing embryo forms. (32) To avoid conception, individuals may choose to explore options for birth control that prevent the female from ovulating (releasing an egg) or prevent the male sperm from reaching the egg.

Forms of birth control
There are numerous types of birth control available, all ranging in safety, length of effectiveness, and ease of accessibility. Determining the best birth control method is a personal choice with many considerations.
Quality supplement plans in less than a minute
Hormonal methods
Hormonal birth control inhibits and/or modulates the natural release of estrogen and progesterone to prevent ovulation on a monthly basis. Hormonal contraceptives are usually well tolerated, reversible, and available via prescription from a physician or other licensed healthcare professional with prescribing rights. Examples of hormonal birth control include:
- Emergency contraception, sometimes referred to as “the morning-after pill” (can be acquired over-the-counter)
- Implants
- Injections
- Oral contraception (the birth control pill)
- Transdermal patches
- Vaginal ring (26)
Long-acting reversible contraception
For a long-term approach, a doctor or healthcare professional may insert an intrauterine device (IUD) into the uterus. IUDs are small T-shaped devices, designed to remain in the uterus for many years. Copper IUDs release copper ions into the surrounding tissue, thereby inhibiting sperm motility. (15) Hormonal IUDs, on the other hand, release small amounts of progestin to create an unsuitable environment for sperm survival and fertilization. (14)
Physical barriers
Physical barriers are used on an as-needed basis, and are usually available over-the-counter. Barriers, such as those listed below, provide a physical obstacle to the successful fertilization of an egg.
- Female diaphragms
- Female sponges, which also contain spermacide to prevent sperm from entering the uterus
- Male condoms (6)
Natural family planning
Natural family planning involves tracking fertility signals throughout the menstrual cycle, such as body temperature, ovulation, or cervical mucus secretion, to determine when to engage in and abstain from intercourse in order to increase or reduce the risk of pregnancy. (17)
Permanent sterilization
Sterilization is a permanent method to prevent pregnancy. These procedures, which are usually irreversible, include:
- Female tubal ligation
- Male vasectomy (2)
In the end, the best birth control method is the one that works best for you. Speak with your integrative healthcare practitioner to review your options.
How do birth control pills work?
The first version of the pill was introduced in 1950 as a way for women to control their menstrual cycle and separate sexual activity from conception. (16)
Birth control pills work by modifying or inhibiting the natural hormones associated with menstruation, thus preventing ovulation and the potential for pregnancy. Estrogen and progesterone are female sex hormones that control and maintain menstruation and pregnancy. (7)
Currently, there are three types of oral contraceptive pills:
- Combined synthetic estrogen-progesterone
- Synthetic progesterone (progestin) only
- The extended-use pill (7)
Since progesterone is the primary hormone responsible for maintaining pregnancy, a progesterone-containing pill essentially “tricks” the body into thinking pregnancy has already occurred and, therefore, prevents the release of an egg during the menstrual cycle. Progesterone also contributes to an unfriendly cervical environment, inhibiting sperm from penetrating through to the uterus. (7)
Typically, the pill is taken orally once a day, in a cyclical dosing format. A prescription usually covers four weeks of pills at a time, with each four-week packet containing one week of hormone-free pills to allow a menses. (13) Used consistently and correctly every time, the birth control pill is very effective with less than one in 100 women becoming pregnant in the first year of use. (7)
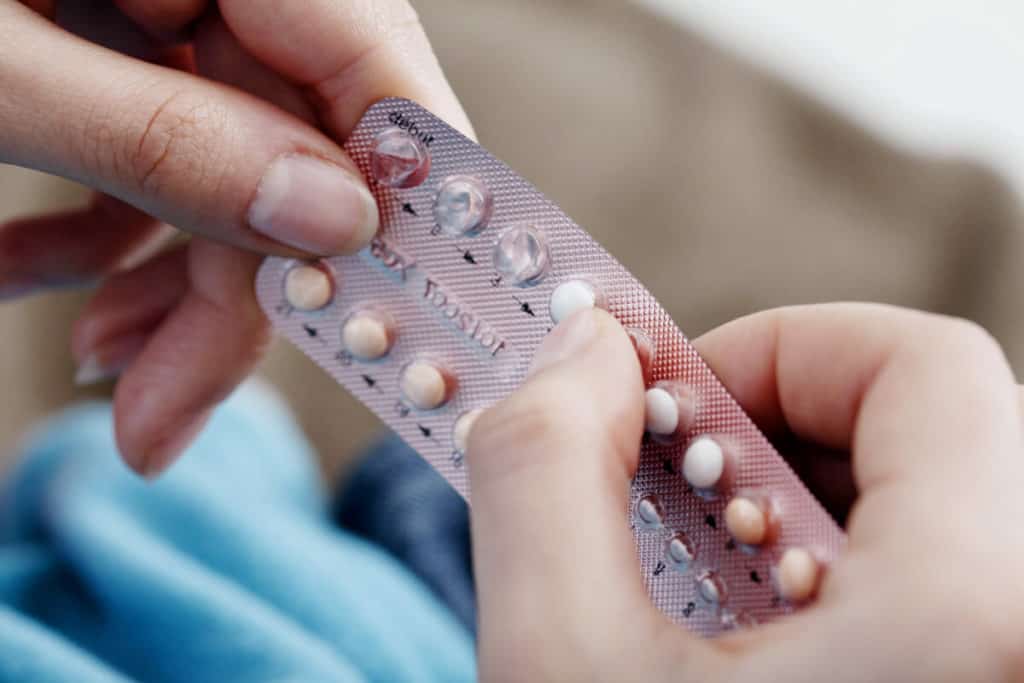
Benefits of the birth control pill
The birth control pill may offer beneficial results to individuals looking for effects beyond pregnancy prevention, including:
- Improvement of hormonal acne
- Management of premenstrual syndrome (PMS) and support for polycystic ovarian syndrome (PCOS)
- Reduced risk of endometrial cancer (5)(19)
- Reduction of menstrual pain
- Reduction of migraines
- Regulation of heavy menstruation

Birth control side effects
Despite its many benefits, there are also many side effects associated with oral contraceptives, including:
- Acne
- Breast tenderness or swelling (10)
- Decreased sexual desire
- Depression (20)
- Headaches
- Increased blood pressure
- Nausea
- Spotting or bleeding in between periods
- Weight gain
Rare but serious potential side effects include stroke and an increased risk of breast cancer, liver tumors, and gallbladder disease. (10)
Contraindications for oral contraceptives
In some instances, the use of the birth control pill should be avoided entirely as it may increase the risk of developing rare complications such as:
- Blood clots
- Deep vein thrombosis
- Heart attack
- Hypertension (high blood pressure) (12)
- Stroke
Smokers over the age of 35 should avoid taking the pill as their risk of cardiovascular events and deep vein thromboembolisms is significantly increased. (7)(16) Women with a history of heart disease, blood clots, (10) or breast and endometrial cancers (7) should also avoid hormonal contraceptive use due to the increased risk of developing serious complications such as those listed above.
Common nutrient depletions associated with “the pill”
Many prescription medications can affect the body’s ability to absorb and utilize nutrients from the diet. Taking the pill is most commonly associated with the following nutrient depletions.

Magnesium
Magnesium has long been recognized as an essential mineral for maintaining good health, proper nerve function, and healthy blood pressure levels. It’s a key nutrient of concern for individuals taking the pill as it is involved in regulating normal blood clotting activity. (25) One study showed that females taking oral contraceptives had significantly lower levels of serum magnesium levels than a control group, potentially increasing their risk of thromboembolism (blood clot). (22)
Another study exploring the relationship between magnesium and estrogen showed that higher estrogen levels, such as those superficially caused by taking hormonal contraceptives, may alter normal blood mineral levels, increasing the risk of blood clots and thrombosis. (30)
Vitamin C
Vitamin C is essential for immune function, collagen formation, and antioxidant protection. Oral contraceptives have been shown to decrease vitamin C concentrations in platelets and blood plasma, negatively affecting how much vitamin C is available for the body’s tissues to uptake. (28)(18)
B vitamins
The B vitamins are a group of vitamins that work together to provide energy and reduce the effects of stress. A review of the literature has indicated that birth control pills can alter various B vitamin levels in the body. (33)
Vitamin B2 (riboflavin) and Vitamin B6 (pyridoxine)
Oral contraceptives may interfere with riboflavin metabolism, (18) increasing the need for consumption of this vitamin through food or supplementation. Further, riboflavin works together with vitamin B6 to reduce the risk of anemia. One study examining the metabolism of B vitamins in a large population of women showed a significant reduction of vitamin B6 in the blood after taking oral contraceptives. (27)
Vitamin B9 (folate)
A 2015 meta-analysis showed that folate status was significantly reduced among oral contraceptive users. (31) Folate is involved in DNA synthesis, repair, and cognitive development. (4)
Vitamin B12 (cobalamin)
A recent study measuring serum B12 levels in women taking oral contraceptives showed a sharp decrease in levels during the first six months of use compared to non-hormonal contraceptive users. (3) Vitamin B12 is needed for energy and proper DNA synthesis. (21)
CoQ10
Coenzyme Q10 (CoQ10) is a well known antioxidant, protecting cells from free radical damage. (29) It is an important nutrient for heart health and the prevention of cardiovascular disease. (24) A 2006 study examined blood samples from 15 women using oral contraceptives for at least six months. It showed that serum levels of CoQ10 were significantly lower during the first part of the menstrual cycle, leading the authors to consider future antioxidant impacts for women taking birth control. (23)
Zinc and copper
These two minerals work in balance to support important biochemical and immune functions in the body. It is well documented that oral contraceptive users typically have elevated blood copper levels. (1) Copper is highly reactive and may lead to oxidative tissue damage if not properly balanced with zinc. (11) A study of 24 women taking oral contraceptives compared zinc and copper levels against a control group who were not taking hormonal birth control. Compared to the control group, zinc levels were significantly lower for the women taking oral contraceptives, while copper levels significantly higher. (9)
The bottom line
The decision to use oral contraceptives is a personal choice with many considerations. Women taking the birth control pill should pay particular attention to vitamin and mineral intake and depletions, as well as speak with their integrative healthcare providers to determine if supplementation is necessary. (33) A thorough review of your medical history in comparison to the benefits and side effects of the pill is also important to determine if the birth control pill is right for you.
Quality supplement plans in less than a minute
- Babi, R., Tariba, B., Kova, J., Pizent, A., Marnai, V.M. & Macan, J. (2013). Relevance of serum copper elevation induced by oral contraceptives: a meta-analysis. Contraception. 87(6), 790-800. Doi: https://doi.org/10.1016/j.contraception.2012.10.006
- Bartz, D., & Greenberg, J. A. (2008). Sterilization in the United States. Reviews in obstetrics & gynecology, 1(1), 23–32. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2492586/
- Berenson, A.B., & Rahman, M. (2012). Effect of hormonal contraceptives on vitamin B12 level and the association of the latter with bone mineral density. Contraception. 86(5), 481-487. Doi: 10.1016/j.contraception.2012.02.015.
- Chan, Y. M., Bailey, R., & O’Connor, D. L. (2013). Folate. Advances in Nutrition (Bethesda, Md.), 4(1), 123–125. Doi: https://doi.org/10.3945/an.112.003392
- Collaborative Group on Epidemiological Studies on Endometrial Cancer. (2015). Endometrial cancer and oral contraceptives: an individual participant meta-analysis of 27,276 women with endometrial cancer from 36 epidemiological studies. The Lancet. 16(9), 1061-1070. Doi: DOI: https://doi.org/10.1016/S1470-2045(15)00212-0
- Colquitt, C.W., & Martin, T.S. (2015). Contraceptive methods: A review of nonbarrier and barrier products. Journal of Pharmacy Practice. 30(1), 130-135. Doi: https://doi.org/10.1177/0897190015585751
- Cooper DB, Mahdy H. Oral Contraceptive Pills. . In: StatPearls . Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK430882/
- Daniels, K., & Abma, J.C. (2018). Current Contraceptive Status Among Women Aged 15-49: United States 2015-2017. NCHS Data Brief No. 327. https://www.cdc.gov/nchs/products/databriefs/db327.htm
- Dorea, J. G., Ferraz, E., & Queiroz, E. F. (1982). . Archivos latinoamericanos de nutricion, 32(1), 101–110. https://pubmed.ncbi.nlm.nih.gov/7181622/
- Frye, C. A. (2006). An overview of oral contraceptives; Mechanism of action and clinical use. Neurology. 66(66 suppl 3). Doi: 10.1212/WNL.66.66_suppl_3.S29
- Gaetke, L.M., & Chow, C.K. (2003). Copper toxicity, oxidative stress, and antioxidant nutrients. Toxicology. 189(1-2), 147-163. Doi: https://doi.org/10.1016/S0300-483X(03)00159-8
- Grossman, D., White, K., Hopkins, K., Amastae, J., Shedlin, M., & Potter, J. E. (2011). Contraindications to combined oral contraceptives among over-the-counter compared with prescription users. Obstetrics and gynecology, 117(3), 558–565. Doi: https://doi.org/10.1097/AOG.0b013e31820b0244
- Jin, J. (2014). Oral contraceptives. Journal of the American Medical Association. 311(3), DOI: doi:10.1001/jama.2013.283505
- Kailasam, C., & Cahill, D. (2008). Review of the safety, efficacy and patient acceptability of the levonorgestrel-releasing intrauterine system. Patient Preference and Adherence, 2, 293–302. Doi: https://doi.org/10.2147/ppa.s3464
- Kaneshiro, B., & Aeby, T. (2010). Long-term safety, efficacy, and patient acceptability of the intrauterine Copper T-380A contraceptive device. International journal of women’s health, 2, 211–220. https://doi.org/10.2147/ijwh.s6914
- Liao, P. V., & Dollin, J. (2012). Half a century of the oral contraceptive pill: historical review and view to the future. Canadian family physician Medecin de famille canadien, 58(12), e757–e760. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3520685/
- Matis, N. (1983). Natural family planning: a birth control alternative. Journal of Nurse-Midwifery. 28(1), 7-16. Doi: https://doi.org/10.1016/0091-2182(83)90239-2
- Matsui, M.S.,& Rozovski, S.J. (1982). Drug-nutrient interaction. Clinical Therapeutics. 4(6), 423-440. https://pubmed.ncbi.nlm.nih.gov/7046936/
- Michels K.A., Pfeiffer R.M., Brinton L.A., & Trabert B. (2018). Modification of the associations between duration of oral contraceptive use and ovarian, endometrial, breast, and colorectal cancers. JAMA Oncology. 4(4), 516-521. doi:10.1001/jamaoncol.2017.4942.
- O’Connell, K., Davis, A.R., & Kerns, J. (2007). Oral contraceptives: side effects and depression in adolescent girls. Contraception. 75(4), 299-304. Doi: https://doi.org/10.1016/j.contraception.2006.09.008
- O’Leary, F., & Samman, S. (2010). Vitamin B12 in health and disease. Nutrients, 2(3), 299–316. Doi: https://doi.org/10.3390/nu2030299
- Olatunbosun, D.A., Adeniyi F.A., & Adadevoh B.K. (1974). Effect of oral contraceptives on Serum magnesium levels. International Journal of Fertility. 19(4), 224-226. https://pubmed.ncbi.nlm.nih.gov/4376539/
- Palan, P. R., Connell, K., Ramirez, E., Inegbenijie, C., Gavara, R. Y., Ouseph, J. A., & Mikhail, M. S. (2005). Effects of menopause and hormone replacement therapy on serum levels of coenzyme Q10 and other lipid-soluble antioxidants. BioFactors (Oxford, England), 25(1-4), 61–66. Doi: https://doi.org/10.1002/biof.5520250107
- Palan, P.R., Magneson, A.T., Castillo, M., Dunne, J. & Mikhail, M.S. (2006). Effects of menstrual cycle and oral contraceptive use on serum levels of lipid-soluble antioxidants. American Journal of Obstetrics and Gynecology. 194(5), e35-e38. Doi: https://doi.org/10.1016/j.ajog.2005.11.032
- Palmery, M., Saraceno, A.V., & Carlomagno, G. (2013). Oral contraceptives and changes in nutritional requirements. European review for medical and pharmacological sciences. 17(13), 1804-1813. PMID: 23852908
- Petitti, D. B., & Sidney, S. (2005). Four decades of research on hormonal contraception. The Permanente Journal, 9(1), 29–34. Doi: https://doi.org/10.7812/tpp/04-129
- Prasad, A.S., Lei, K.Y., Moghissi, K.S., Stryker, J.C., & Oberleas, D. (1976). Effect of oral contraceptives on nutrients. III. Vitamins B6, B12, and folic acid. American Journal of Obstetrics and Gynecology. 125(8), 1063-1069. Doi: 10.1016/0002-9378(76)90809-7
- Rivers, J.M. (1975). Oral contraceptives and ascorbic acid. American Journal of Clinical Nutrition. 28(5), 550-554. Doi: 10.1093/ajcn/28.5.550.
- Saini R. (2011). Coenzyme Q10: The essential nutrient. Journal of Pharmacy & Bioallied Sciences, 3(3), 466–467. Doi: https://doi.org/10.4103/0975-7406.84471
- Seelig, M.S. (1993). Interrelationship of magnesium and estrogen in cardiovascular and bone disorders, eclampsia, migraine and premenstrual syndrome. Journal of the American College of Nutrition. 12(4), 442-458. Doi: 10.1080/07315724.1993.10718335.
- Shere, M., Bapat, P., Nickel, C., Kapur, B., & Koren, G. (2015). Association Between Use of Oral Contraceptives and Folate Status: A Systematic Review and Meta-Analysis. Journal of Obstetrics and Gynaecology Canada. 37(5), 430-438. Doi: 10.1016/S1701-2163(15)30258-9
- Stephenson, J., Heslehurst, N., & Hall, J., et al. (2018). Before the beginning: nutrition and lifestyle in the preconception period and its importance for future health. Lancet (London, England), 391(10132), 1830–1841. Doi: https://doi.org/10.1016/S0140-6736(18)30311-8
- Webb, J.L. (1980). Nutritional effects of oral contraceptive use: a review. The Journal of Reproductive Medicine. 25(4), 150-155. https://pubmed.ncbi.nlm.nih.gov/7001015/
- World Health Organization. (1975). Advances in methods of fertility regulation. https://apps.who.int/iris/bitstream/handle/10665/38635/WHO_TRS_575.pdf?sequence=1&isAllowed=y





