What is histamine?
Histamine is a compound that is formed through the metabolism of certain amino acids. Varying levels of histamine are found naturally in the foods we consume. It is also produced by the body, where it is stored in certain immune cells, including mast cells and basophils. (7) Histamine is released from these cells during allergic and other immune responses. (7)(8) Consuming large quantities of histamine, over 100 mg, may result in a mild adverse reaction, while higher amounts over 1000 mg may lead to histamine intoxication, also referred to as histamine poisoning. (8)
What is histamine intolerance?
Under typical conditions, histamine, released in the body or ingested through food, is broken down by two enzymes: histamine-N-methyltransferase (HNMT) and diamine oxidase (DAO). (6)(8) High levels of histamine may occur in individuals with reduced activity of these enzymes. When levels of histamine are increased and/or the ability to break down histamine is impaired, an individual may experience histamine intolerance, which generally presents as an allergic reaction. (6)
What causes histamine intolerance?
Certain individuals may have an increased sensitivity to biogenic amines such as histamine. Factors that have been associated with an increased risk of histamine intolerance include:
- Certain medications that may inhibit the activity of histamine-degrading enzymes (e.g., acetylcysteine, metamizole, metoclopramide, metronidazole, verapamil)
- Certain health conditions (e.g., coronary heart disease, hypertension, respiratory diseases)
- Gastrointestinal conditions (e.g., Crohn’s disease, gastric and colon ulcers, gastritis, irritable bowel syndrome)
- Vitamin B12 deficiency (7)(8)
Mast cell conditions that increase the secretion of histamine are also commonly associated with symptoms of histamine intolerance. Mast cells, found throughout the body, are cells involved in the innate immune response and are the primary source of histamine in the intestines. (7) When specific immune receptors detect a foreign substance in the body, mast cells secrete inflammatory compounds such as histamine as a protective response. (3) Mast cell activation is characterized by increased plasma and urine histamine levels, and increased histamine metabolites in urine.
Several conditions are associated with mast cell activation, including:
- Allergies mediated by immunoglobulin-E (IgE) and other hypersensitivities
- Atopic conditions
- Mastocytosis
- Primary mast cell disorders (7)
Signs and symptoms of histamine intolerance
Histamine intolerance symptoms present as an allergic response and may include:
- Arrhythmia
- Asthma
- Diarrhea
- Flushing
- Headache
- Hypotension
- Symptoms of rhinoconjunctivitis (e.g., nasal congestion, post-nasal drip, sneezing)
- Pruritus (e.g., itchy skin)
- Urticaria (e.g., hives) (6)

Histamine-free diet: an therapeutic approach to histamine intolerance
Dietary support for histamine intolerance may involve a histamine-free diet. (4)(6) A study examined the effects of a four-week histamine-free diet intervention in 22 adults with chronic urticaria (CU). CU is a common skin condition characterized by episodes of red marks and swelling which last longer than six weeks. (10) The study found that, compared to baseline, plasma histamine levels were significantly reduced following adherence to the diet. Additionally, urticaria severity score (USS) and urticaria activity score (UAS) both decreased following the intervention. This suggests that a histamine-free diet may help improve symptoms associated with dietary histamine intake or histamine intolerance, such as CU. (10) Research also suggests that following a histamine-reduced diet may increase levels of the DAO enzyme. A group of individuals diagnosed with histamine intolerance followed a low histamine diet for an average of 13 months. Results demonstrated that increased levels of DAO were correlated with the degree of compliance to the diet. (5) After eliminating high-histamine and histamine-liberating foods, individual tolerance levels can be determined by slowly reintroducing foods to test for potential reactions. (7) Certain foods may increase levels of histamine by providing a dietary source of histamine, or by liberating histamine in the body. It’s important to note that studies have found inconsistent levels of histamine in various foods. (7) Histamine levels may fluctuate based on the maturity, storage, and processing of the food. (8) However, the following table may be used as a general guideline of foods to avoid on a histamine-free diet.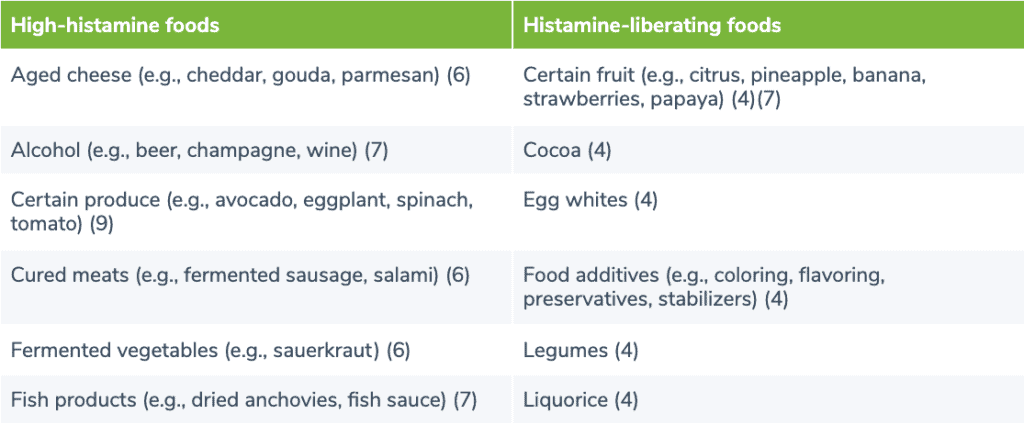
The bottom line
Some individuals with histamine intolerance may benefit from taking antihistamine medication or a DAO supplement. (4)(7) Additionally, certain nutrients, including copper, (4) vitamin B6, and vitamin C, may help to support histamine degradation. (7) If you suspect you may have histamine intolerance, speak with your integrative healthcare practitioner about incorporating a histamine-free diet and these nutrients into your wellness plan.Help more patients.
right in your Fullscript account!
New to Fullscript? Sign up now.
- Chung, B. Y., Park, S. Y., Byun, Y. S., Son, J. H., Choi, Y. W., Cho, Y. S., … Park, C. W. (2017). Effect of different cooking methods on histamine levels in selected foods. Annals of Dermatology, 29(6), 706–714.
- Dougherty, J. M., Alsayouri, K., & Sadowski, A. (n.d.). Allergy. In Stat Pearls . Treasure Island, FL: StatPearls Publishing. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK545237/
- Fong, M., & Crane, J. S. (2019). Histology, Mast Cells. In StatPearls . Treasure Island, FL: StatPearls Publishing. Retrieved from https://www.ncbi.nlm.nih.gov/books/NBK499904/
- Kovacova-Hanuskova, E., Buday, T., Gavliakova, S., & Plevkova, J. (2015). Histamine, histamine intoxication and intolerance. Allergologia Et Immunopathologia, 43(5), 498–506.
- Lackner, S., Malcher, V., Enko, D., Mangge, H., Holasek, S. J., & Schnedl, W. J. (2018). Histamine-reduced diet and increase of serum diamine oxidase correlating to diet compliance in histamine intolerance. European Journal of Clinical Nutrition, 73(1), 102–104.
- Maintz, L., & Novak, N. (2007). Histamine and histamine intolerance. The American Journal of Clinical Nutrition, 85(5), 1185–1196.
- Martin, I. S. M., Brachero, S., & Vilar, E. G. (2016). Histamine intolerance and dietary management: A complete review. Allergologia Et Immunopathologia, 44(5), 475–483.
- Reese, I., Ballmer-Weber, B., Beyer, K., Fuchs, T., Kleine-Tebbe, J., Klimek, L., … Worm, M. (2017). German guideline for the management of adverse reactions to ingested histamine: Guideline of the German Society for Allergology and Clinical Immunology (DGAKI), the German Society for Pediatric Allergology and Environmental Medicine (GPA), the German Association of Allergologists (AeDA), and the Swiss Society for Allergology and Immunology (SGAI). Allergo Journal International, 26(2), 72–79.
- Sánchez-Pérez, S., Comas-Basté, O., Rabell-González, J., Veciana-Nogués, M. T., Latorre-Moratalla, M. L., & Vidal-Carou, M. C. (2018). Biogenic Amines in Plant-Origin Foods: Are They Frequently Underestimated in Low-Histamine Diets? Foods, 7(12), 205.
- Son, J. H., Chung, B. Y., Kim, H. O., & Park, C. W. (2018). A histamine-free diet is helpful for treatment of adult patients with chronic spontaneous urticaria. Annals of Dermatology, 30(2), 164–172.




